Gingival Atrophy/Telangiectasia
Gingival atrophy and recession have been thought to be a result of oral GVHD. However, this is rarely documented as biopsy of the thinned gingiva would result in more loss of attached gingiva. It may be totally asymptomatic but most patients will complain of tooth sensitivity to cold stimuli and to brushing. With loss of the interdental papilla, “black” spaces between the teeth may be the only chief complaint. Although the gingiva do not recover, this is usually self-limiting. Periodontal surgical procedures may be contemplated when the GVH has resolved. The following are examples which show a very thinned gingiva with virtually no stippled attached gingiva. Recession to expose cervical roots appears to be accelerated and the underlying vasculature appears quite prominent.
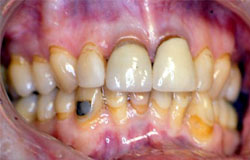
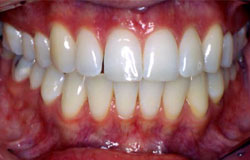
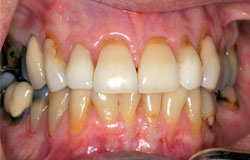
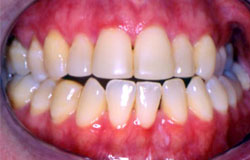
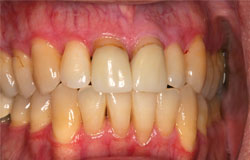
Gingival erythema
In the following examples, irregular but generalized gingival erythema is seen. The first two cases are asymptomatic but have remained unchanged in appearance for several years post transplant.
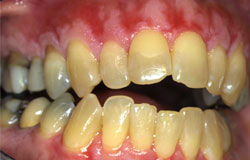
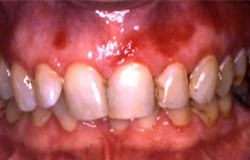
The next two examples show irregular red patches as well but in these cases, there is pain with brushing and eating acidic or spicy foods. Toothpastes without sodium lauroyl sulfate are recommended for this type. Oral hygiene is extremely important to reduce the added inflammation of bacterial plaque. These are examples of chronic GVH of the gingiva.
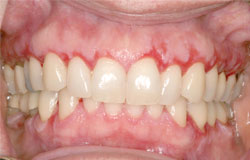
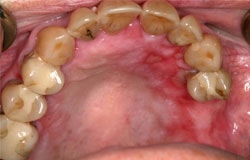
These 2 clinical photographs are examples of acute GVH of the gingiva. Topical steroids would be indicated if symptomatic.
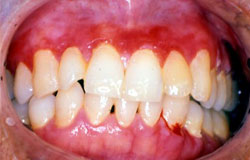
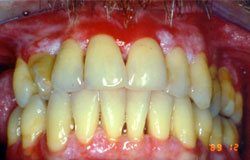
The oral lesions of GVHD may have significant impact on his oral/dental health and include xerostomia, (which would predispose to caries), atrophy of the gingiva and oral mucosal lichenoid lesions with or without ulceration.